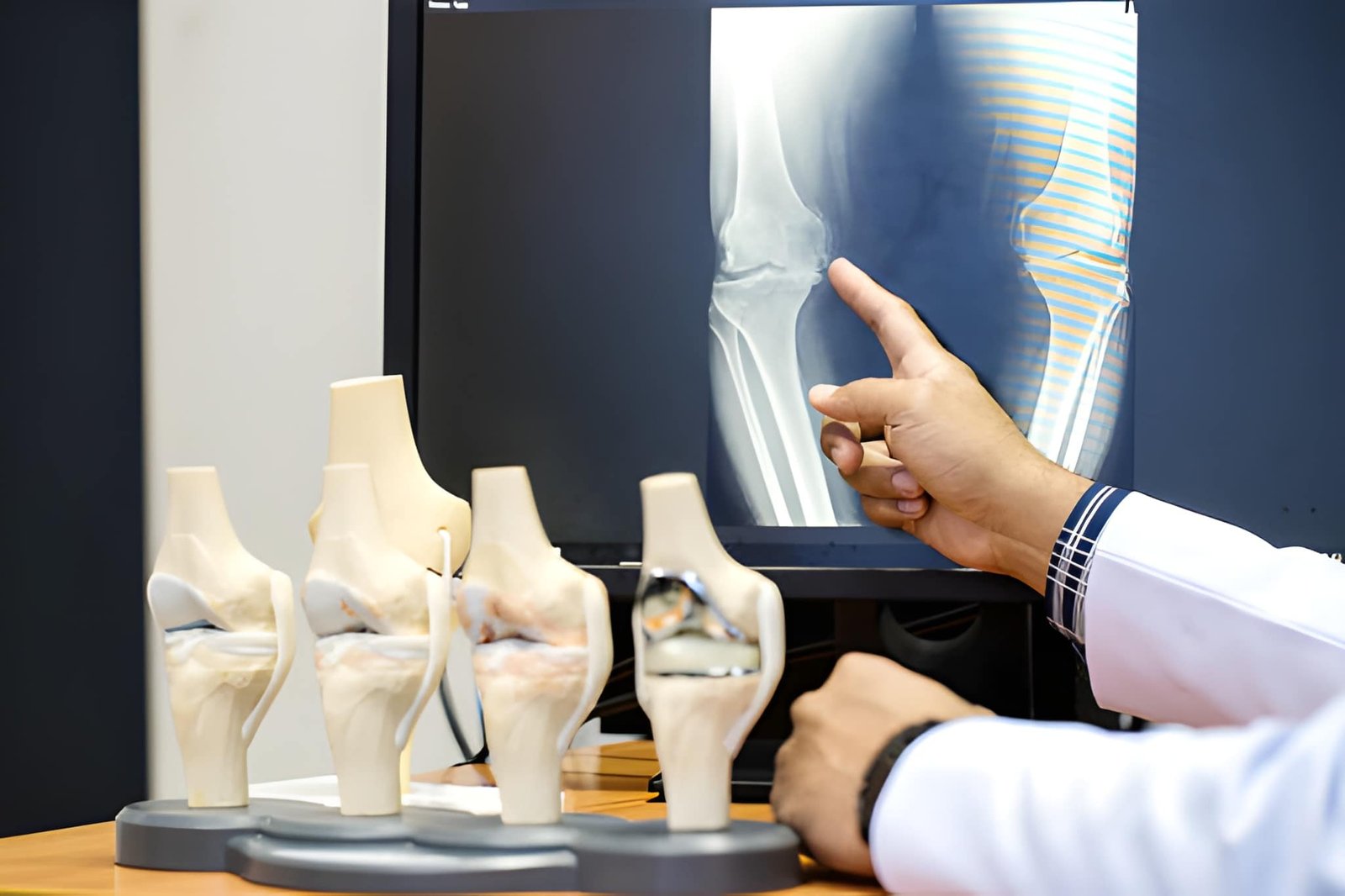
One of the most frustrating conversations in an orthopaedic clinic goes like this: the patient walks in with knee pain that’s affecting sleep, stairs, and daily life. The X-ray report says “normal.” And yet, the pain is very real. According to Dr Udayan Das, the best orthopaedic doctor in Bhubaneswar, this mismatch between reports and reality is far more common than people think, and it’s one of the biggest reasons patients delay the right treatment. The truth is, an X-ray only tells part of the story. It’s excellent at showing bones, joint space narrowing, and advanced arthritis. But knees are more than bones. Pain often begins long before damage becomes visible on an X-ray. One common culprit is early cartilage wear. In the initial stages of osteoarthritis, cartilage softens and thins unevenly. This stage can be extremely painful, especially during walking or prolonged standing, but it often looks “normal” on X-ray. Many patients are told, “Nothing is wrong,” when in reality, something is clearly starting. Then there are ligament and meniscus injuries, especially in people who squat frequently, climb stairs daily, or play weekend sports. A small meniscal tear or ligament strain can cause sharp pain, locking, or instability, but none of it appears on a plain X-ray. This is where patients feel dismissed, even though their symptoms are classic. Another overlooked factor is patellofemoral pain, pain originating from the kneecap. This often affects young adults, office workers, and women. The knee looks perfect on imaging, but pain flares up while climbing stairs, sitting cross-legged, or getting up from the floor. Without a proper clinical examination, it’s easy to miss. Dr Udayan Das often points out that muscle imbalance and biomechanics play a huge role. Weak quadriceps, tight hamstrings, poor posture, or altered walking patterns can overload the knee joint. The X-ray stays clean, but the knee keeps protesting. There’s also a common patient mistake: self-medicating after a “normal” report. Painkillers may temporarily mask symptoms, but the underlying problem continues to progress quietly. By the time changes show up on X-ray, damage is often more advanced and harder to reverse. What actually helps in these cases is not just another report, but a proper clinical assessment, watching how the patient walks, checking alignment, testing joint stability, and understanding lifestyle factors. Sometimes an MRI is needed; sometimes targeted physiotherapy does more than any pill. The biggest takeaway? A normal X-ray does not mean imaginary pain. It simply means the problem hasn’t declared itself on bone yet. For patients struggling with unexplained knee pain, early evaluation by an experienced specialist like Dr Udayan Das, the best orthopaedic doctor in Bhubaneswar, can make the difference between timely correction and long-term damage. Pain is information. Ignoring it just because a report looks fine is the real mistake.